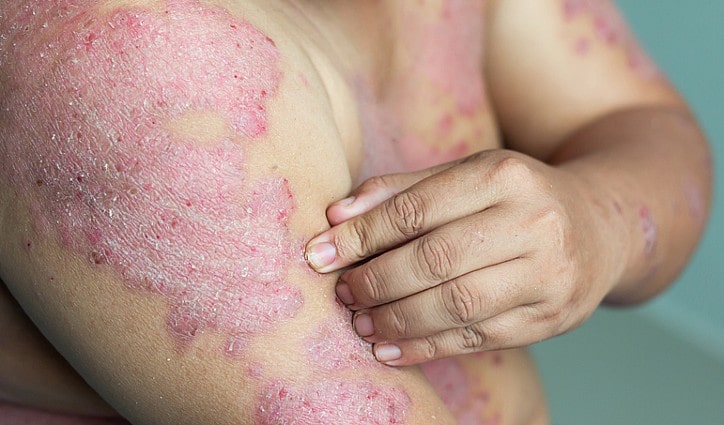
Is that itch on your skin merely rashes, or more than that?
Scabies is a skin infestation caused by the microscopic human itch mite. There are nearly 130 million scabies cases globally. The miniature scabies mite burrows into the upper-most layer of the skin where it resides and lays its eggs. Sounds scary? Don’t worry, it’s not half as bad as you think — this article will take you through everything you need to know about scabies, including its symptoms and treatment options in Singapore.
How is scabies transmitted?
Even though scabies is an extremely contagious condition and can easily be transmitted from one individual to another, scabies is not a sexually transmitted disease. Scabies infection is triggered by the Sarcoptes scabies parasite. Although I mentioned that scabies is not a sexually transmitted disease, it can however be transmitted via sexual contact. Of course, this is not usually the case among children with scabies. For children, the infestation of mites may be transmitted through infested bedding or clothing. So, this implies that intimate contact isn't necessary in order for scabies to spread.
When you get infected with the Sarcoptes scabiei parasite, it will take a few weeks for your body to acclimatise. During this period, you may only experience intense itch, a classic symptom of scabies. However, if you are suffering from a reinfection of scabies, your itch symptoms will develop a lot faster than usual — usually within the first 24 hours.. This is because with reinfection, your body has already been sensitized by the parasite.
So, what are some of the most common scabies symptoms?
The most common symptoms of scabies are:
- Itching, which usually worsens at night
- Rashes — this usually occurs nearly anywhere on the body except your head, but typically the rash happens on the web spaces of your toes, fingers, groin as well as the genital region. How can you differentiate the rash from rabies to regular rashes? Well, scabies rashes are usually characterized by silvery linings or trail-like lines that are also referred to as burrows. It is worth mentioning that rashes are often confused with eczema which doesn't disappear.
- Rashes on the head. Individuals with compromised immune systems —especially the elderly and children— usually experience scabies rashes on their head. We often refer to this as crusted scabies or Norwegian Scabies.
What does the term crusted scabies mean?
As earlier mentioned, crusted scabies is a severe type of scabies that can occur among individuals with compromised immune systems, disabled or debilitated people, or the aged. It is also referred to as Norwegian scabies. Those suffering from crusted scabies usually experience thick crusts of skin that are filled with numerous scabies mites as well as eggs.
Crusted scabies are extremely contagious. Patients with crusted scabies can easily spread the disease to others through both skin-to-skin contact and contamination of vital items such as furniture, bedding, and clothing. Most importantly, people with crusted scabies usually do not exhibit the typical symptoms of scabies, such as itching or the characteristic rash.
I must emphasise that those suffering from crusted scabies should always seek immediate and highly aggressive medical intervention to ensure they don't cause scabies outbreaks. Those who have a compromised immune system — such as those with HIV or lymphoma as well as those suffering from long-term steroid use— are more prone to crusted scabies.
What are some of the treatment options for scabies infections?
Even though scabies can be a highly worrisome condition, it can be eliminated effectively through treatment. A topical medication known as Permethrin is usually applied as a single dose to the entire skin, from your scalp down to your toes. On most occasions, a single dosage is enough to eradicate symptoms. Another medication, an antiparasitic agent known as Ivermectin may equally be administered orally to completely eradicate scabies. After successful treatment, you should thoroughly wash all your contaminated bedding and clothing using hot water.
I should also add that HIV may put you at a greater risk of developing widespread scabies, usually described as Crusted Scabies.
What extra precautionary measures should I take after scabies treatment?
To ensure you do not get reinfected with scabies again, I recommend the following:
- Thoroughly launder your bedding, linen as well as clothing at high temperatures of at least 50 degrees.
- If you have any clothes that are not washable, you should put them inside sealed bags for three days until all the scabies mites die.
- Get screened for other sexually transmitted infections such as HIV, since HIV increases your risk of developing scabies.
- Practice good personal hygiene, such as keeping your fingernails short and trimmed to avoid skin infections which may occur as a result of excessive scratching.
- If you have a special partner or very close household members, they should be treated within the first month preceding scabies infestation.
- Abstain from intercourse until you as well as your partners have been treated.
Why is it important to treat scabies?
As previously explained, scabies is spread through direct, extended, skin-to-skin contact with an already infected individual. Generally, the contact must be a prolonged one — so a quick handshake or hug will not result in the spread of scabies. Regardless, scabies is usually spread quite easily among sexual partners as well as household members. It is also important to mention that in most adult scabies cases I’ve seen, the infection is on most occasions spread through sexual intercourse.
At times, scabies is transmitted indirectly through the sharing of items such as towels, clothing, or bedding used by an already infected person. In scenarios where the infected individual suffers from crusted scabies, the indirect spread will occur quite easily.

How long does scabies last?
Many patients ignore treatment for scabies as they often think the rash will disappear on their own. However, without treatment, your scabies will not heal. Additionally, those who seek treatment within 24 hours of obtaining the infection will no longer be contagious.
When do scabies-related symptoms appear after an infestation?
If you have never suffered from scabies before, it may take between four to eight weeks for your symptoms to develop. However, even during this period of dormancy, you can still spread scabies. On the other hand, if you have had scabies before, your symptoms will appear between one to four days after initial exposure.
So, how long do scabies live?
If you didn't know, scabies mites can reside in your body for as long as one or two months. Outside your body, scabies mites will not survive more than three days. It is also crucial to mention that scabies mites usually die when exposed to a temperature of at least 50 degrees for ten minutes — hence why it’s so important to thoroughly wash your bedding in high heat!
Can I be fully cured of scabies?
Yes, of course! Effective treatment will completely eradicate scabies off your body. Products used in the treatment of scabies are known as scabicides simply because they eradicate scabies mites — some of them also kill scabies eggs.
It is very important to note that scabicides used to treat human scabies are only available with the prescription of a doctor. You are highly encouraged to always follow your doctor's prescription. If your symptoms persist even after treatment —typically more than four weeks after treatment— your doctor may consider retreatment.
Who else should be treated for scabies?
Anybody who is diagnosed with scabies should get treated for scabies. This includes your sexual partners, household members and other contacts who may have had direct and extended skin-to-skin contacts with you. They should get treated as soon as possible. To ensure no one in the same household suffers reinfection, everyone at home should get treated at the same time.
Can my pet infect me with scabies?
Fortunately, you will not get scabies from your pet. This is because animals don't transmit human scabies. Animals can become infected with a totally different type of scabies mite that doesn't survive on humans at all!
Who can get scabies?
Anyone can become infected with scabies. Scabies mites will attack you regardless of your race, gender, social class, or even income level. Getting mites equally doesn't have anything to do with the level of your hygiene. Anybody's skin is an inviting place for a mite looking for a place to burrow!
How is scabies diagnosed?
On most occasions, your doctor will diagnose scabies by simply conducting a physical examination and inspecting the affected skin area. However, in some instances, your doctor might want to verify the diagnosis by removing a mite from your skin using a needle. Your doctor can also scrap the burrows to determine the presence of scabies mites and their eggs.
While scabies infestation may not pose a serious health problem, it is an irritating and potentially embarrassing health condition. It is also a highly contagious condition, which is why immediate treatment should be seeked for yourself and the whole group of persons who have been in regular contact with you.
References
- Leung, A., Lam, J. M., & Leong, K. F. (2020). Scabies: A Neglected Global Disease. Current pediatric reviews, 16(1), 33–42. https://doi.org/10.2174/1573396315666190717114131
- Chouela, E., Abeldaño, A., Pellerano, G., & Hernández, M. I. (2002). Diagnosis and treatment of scabies: a practical guide. American journal of clinical dermatology, 3(1), 9–18. https://doi.org/10.2165/00128071-200203010-00002This article was written and medically reviewed by Dr Ben, M.D on 28/05/2021Leung, A., Lam, J. M., & Leong, K. F. (2020). Scabies: A Neglected Global Disease. Current pediatric reviews, 16(1), 33–42. https://doi.org/10.2174/1573396315666190717114131
- Chouela, E., Abeldaño, A., Pellerano, G., & Hernández, M. I. (2002). Diagnosis and treatment of scabies: a practical guide. American journal of clinical dermatology, 3(1), 9–18. https://doi.org/10.2165/00128071-200203010-00002
This article was written and medically reviewed by Dr Ben, M.D on 08/05/2021